Working on combat veterans in Ukraine. What I learned.
How structural integration helped veterans with amputations, and what it taught me about the body's capacity to heal.
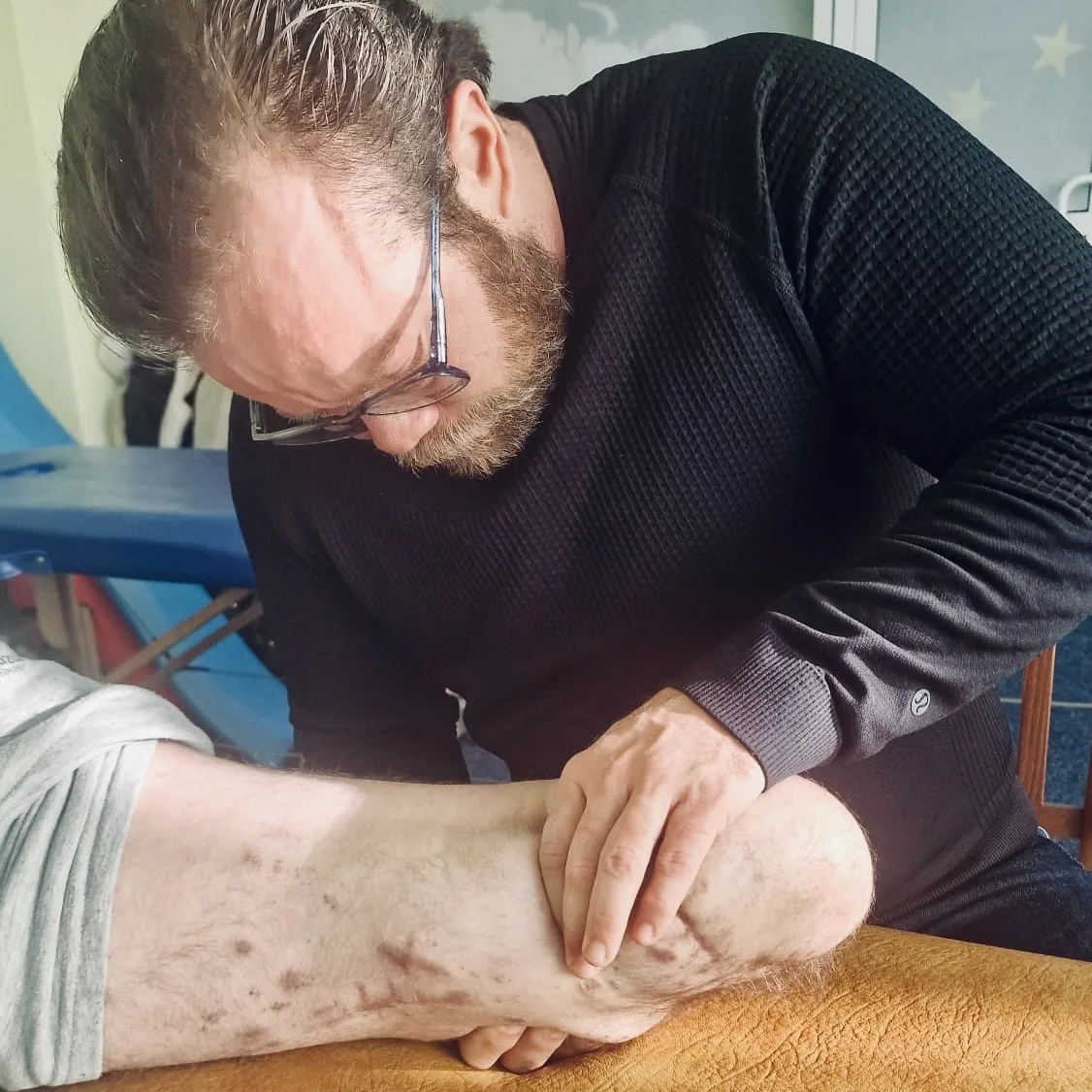
There are moments in your career that redefine everything you thought you knew about the work you do. For me, that moment came in Ukraine, kneeling beside a young veteran who had lost both legs below the knee, feeling the dense, fibrous scar tissue beneath my hands and realizing that everything I had ever learned about structural integration was about to be tested in ways I never imagined.
I traveled to Ukraine twice to assist Sharon Wheeler, a master structural integration practitioner with over fifty years of experience and a pioneer in scar tissue work. Sharon had organized a volunteer program to work with combat veterans dealing with amputations and severe injuries from the ongoing conflict. When she asked if I wanted to assist, I did not hesitate. I knew this was the kind of work that would push me to grow, and that these were people who desperately needed what structural integration could offer.
The Reality on the Ground
Nothing fully prepares you for what it is like to walk into a room of young men and women who have lost limbs in combat. Many of them were in their twenties. Some had lost one leg, others both. Several had lost arms. Nearly all of them were dealing with the compounding effects of prosthetic use on a body that was never given the chance to properly heal or reorganize after catastrophic injury.
The standard medical approach for these veterans was focused on survival and basic rehabilitation: stabilize, fit a prosthetic, learn to walk again. But the deeper structural consequences of amputation, the way scar tissue distorts fascial relationships, the compensatory patterns that develop when someone learns to move on a prosthetic without any attention to whole-body organization, those issues were largely unaddressed. That is where we came in.
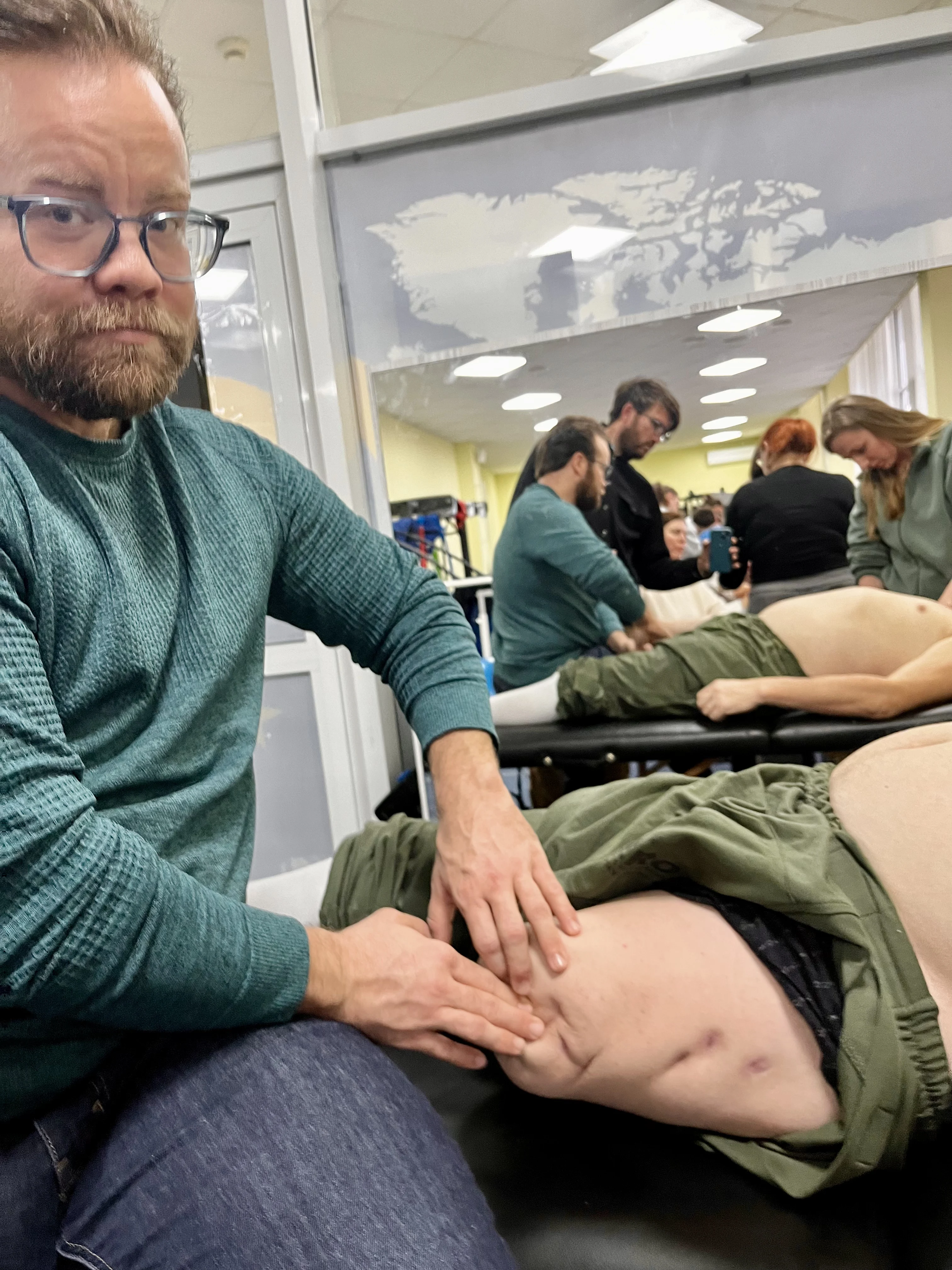
What struck me immediately was the sheer density of the scar tissue. Surgical scars from amputation are not like anything you encounter in a typical practice. The tissue is thick, layered, and often adhered to bone. It restricts movement, creates pain at the prosthetic interface, and sends compensatory strain patterns radiating through the entire body. A veteran who lost a leg below the knee might present with hip dysfunction, low back pain, shoulder tension, and headaches, all traceable back to how that scar tissue was organizing their structure.
Adapting Structural Integration for Scar Tissue and Prosthetics
Working under Sharon's guidance, I learned how to approach scar tissue with a specificity and patience that goes beyond standard structural integration techniques. Sharon's scar tissue work is remarkable. She has developed methods for engaging the layers of scar tissue in a way that allows them to soften, differentiate, and begin to integrate with the surrounding fascial network rather than acting as a rigid, isolated mass.
The key insight was that scar tissue is not the enemy. It is the body's attempt to repair itself, and it responds to intelligent, skilled touch. By working slowly and precisely, layer by layer, we could help the tissue reorganize. Veterans who had been in constant pain at their prosthetic socket would experience immediate relief. Tissue that had been rock-hard would begin to soften and become pliable. Range of motion at nearby joints would improve, sometimes dramatically, within a single session.
We also had to think about the whole body in relation to the prosthetic. When someone walks on a prosthetic leg, the forces traveling through their body are fundamentally different from natural gait. The remaining tissues have to absorb and distribute loads they were never designed to handle in that way. Structural integration gave us the framework to address these compensatory patterns systematically, working through the myofascial lines to help the body find a more efficient and less painful way to organize itself around the prosthetic.

The Power of Touch for Trauma Survivors
Perhaps the most profound lesson from this work had nothing to do with technique. It was about the simple, radical act of touching someone with care and intention when their body has become a source of pain and loss.
Many of these veterans had not been touched in a therapeutic, non-medical way since before their injuries. The medical system had touched them to treat wounds, to fit prosthetics, to assess function. But no one had touched them in a way that communicated: your body still has value, it can still change, it is not broken beyond repair.
I watched hardened combat veterans soften and sometimes weep on the table, not from pain, but from the sheer relief of being met with that kind of attention. Touch, when it is skilled and intentional, communicates something that words cannot. It tells the nervous system that safety is possible. It tells the tissues that reorganization is allowed. For people carrying both physical and psychological trauma, that message can be transformative.
What This Taught Me About the Body's Resilience
Working in Ukraine fundamentally changed how I understand the body's capacity to heal and adapt. I saw tissue change that I would not have believed possible if I had not felt it under my own hands. Scar tissue that had been rigid for months began to soften within minutes of skilled engagement. Veterans who had been told they would always have pain at their prosthetic site found relief. Bodies that had been locked in protective guarding patterns began to open and reorganize.
This experience reinforced something I already believed but now know at a deeper level: the body wants to heal. Given the right input, the right quality of touch, and a practitioner who understands the fascial system as an interconnected whole, the body will move toward better organization. It does not matter how severe the injury or how long the pattern has been in place. Change is always possible.
I also came away with a renewed sense of purpose. I gave a webinar for Anatomy Trains called "Being of Service: Taking Your Practice Into the World" to share what I learned and to encourage other practitioners to find ways to bring their skills to people who need them most. The work we do in our practices is valuable, but when you take it into a context like this, you see its full power.
Bringing It Home
The skills I developed in Ukraine, working with extreme scar tissue, adapting techniques for dramatically altered anatomy, understanding how trauma lives in the tissues, these are skills I bring to every session in my Santa Cruz practice. Whether you are dealing with a surgical scar, recovering from an injury, or carrying the physical imprint of a difficult experience, the principles are the same: the body can reorganize, tissue can change, and skilled touch can catalyze profound healing.
If there is one thing Ukraine taught me, it is that we should never underestimate what the body is capable of, or what compassionate, knowledgeable hands can do to help it get there.